Abstract
Background: The COVID-19 pandemic has brought immense disruption worldwide, dramatically altering the ways we live, work and learn on a day-to-day basis; however, few studies have investigated this from the perspective of primary care providers. In this study, we sought to explore the experiences of primary care providers in the province of Nova Scotia, with the intention of understanding the impact of the COVID-19 pandemic on primary care providers’ ability to provide care, their information pathways, and the personal and professional impact of the pandemic.
Methods: We conducted an exploratory qualitative research study involving semistructured interviews conducted via Zoom videoconferencing or telephone with primary care providers (physicians, nurse practitioners and family practice nurses) who self-identified as working in primary health care in Nova Scotia from June 2020 to April 2021. We performed a thematic analysis involving coding and classifying data according to themes. Emergent themes were then interpreted by seeking commonalties, divergence, relationships and overarching patterns in the data.
Results: Twenty-four primary care providers were interviewed. Subsequent analysis identified 4 interrelated themes within the data: disruption to work–life balance, disruptions to “non-COVID-19” patient care, impact of provincial and centralized policies, and filtering and processing an influx of information.
Interpretation: Our findings showed that managing a crisis of this magnitude requires coordination and new ways of working, balancing professional and personal life, and adapting to already implemented changes (i.e., virtual care). A specific primary care pandemic response plan is essential to mitigate the impact of future health care crises.
The COVID-19 pandemic has brought immense disruption worldwide, dramatically altering the ways we live, work and learn on a day-to-day basis. Health care systems have experienced tremendous impact, caused by gaps in critical knowledge, staffing shortages, and the psychological and social impact on patients1 and health care professionals.2 Public health policies and recommendations resulted in nonessential health services being cancelled or delayed,3,4 disruptions in continuity of care for patients with chronic conditions5–7 and heightened reliance on virtual care.8 The pandemic not only forced changes to patient care, it influenced the lives and practices of primary care providers, including their personal and family well-being.9 Although the impact of the pandemic has been investigated in many areas of medicine,10,11 there remains a need to investigate, from the perspective of primary care providers (e.g., physicians; nurse practitioners; registered nurses, such as family practice nurses; social workers; pharmacists; and other health professionals), the impact the pandemic has had on their practice, their patients and themselves.12–14
Since the province of Nova Scotia declared a state of emergency on Mar. 22, 2020,12 primary care providers have responded to rapidly changing public health measures. The experiences of primary care providers during the early phases of the pandemic may provide insight into the primary care response and the impact of a major health emergency. The objectives of this study were, therefore, to better understand the impact of the onset of the COVID-19 pandemic on primary care providers’ ability to provide care, their information pathways (i.e., how information about COVID-19 was accessed and shared) and the personal and professional impact of the pandemic. The overall program of research investigated the impact across multiple primary care providers. In this article, we report data from the first round of recruitment, which included family physicians, nurse practitioners and family practice nurses, collectively referred to as primary care providers.
Methods
Nova Scotia is a province on the east coast of Canada with governance over its health system via a single health authority (Nova Scotia Health with 4 geographic zones) and a large health centre responsible for women and children’s health that serves 3 provinces. Nova Scotia Health is responsible for the day-to-day delivery of health care in the 4 health regions, 3 of which are primarily rural, whereas the Nova Scotia government’s Department of Health and Wellness is responsible for strategic planning, standards and priority setting.13 Primary care is provided within the provincial health authority and via private practices. As of October 2021, there were 96 collaborative family practice teams in Nova Scotia, which included 409 family doctors, 104 nurse practitioners and 80 registered nurses.14 Most physicians are remunerated through a fee-for-service payment structure,15 and nurses are salaried.16
Nova Scotia announced its first case of COVID-19 on Mar. 15, 2020; 7 days later the government declared a state of emergency, which restricted individual movement to essential reasons and limited travel to and from the province.17 These measures, among others, were implemented to help limit the number of infections during wave 1.
Research design
We used an exploratory qualitative research design, using an inductive approach and involving semistructured 1-on-1 interviews18 to investigate experiences of Nova Scotian primary care providers during the early months of the COVID-19 pandemic. The Consolidated Criteria for Reporting Qualitative Research Checklist guided reporting.19,20
Participants
Purposive sampling of primary care providers was done through each author’s professional contacts and targeted newsletters and listservs of local organizations (e.g., Dalhousie University’s Faculty of Health and School of Nursing email lists, Nova Scotia Health’s newsletters and the Department of Family Medicine newsletter) with the goal of recruiting 25–30 primary care providers. All participants independently contacted the research team. Research staff sent interested participants study information and a consent form. Participants had the opportunity to ask questions via email and answered 3 questions to guide recruitment. A sampling matrix tracked participant discipline, age and geographic location of practice (based on 4 provincial health authority zones). The matrix informed recruitment strategies to achieve a disciplinary and geographically balanced sample. There were no specific exclusion criteria. All participants provided informed, voluntary, oral consent at the beginning of the remote interview.13,17
Data collection
The research team developed a semistructured interview guide (Appendix 1, available at www.cmajopen.ca/content/11/2/E274/suppl/DC1) through discussion to ensure questions aligned with the project objectives of exploring the perspectives and experiences of primary care providers during the first wave of the pandemic. The guide was organized into 3 sections: the perceived impact of the COVID-19 pandemic on the primary care system; access to information, sharing and disseminating information; and personal impact of the pandemic. Questions were designed to elicit details of experiences to ensure a holistic account was recalled. The guide was then pilot-tested to ensure relevant topics were covered while also leaving opportunity for participant-driven narrative and insights. No changes were made after pilot interviews.
Interviews were conducted between June 2020 and April 2021 by 5 research staff, including 3 authors (M.E., E.A.F. and S.K.J.) with previous experience conducting qualitative interviews. One person, who was a research staff member and a patient representative, left the project after data collection and chose not to be included as an author. Each participant completed a single, individual, semistructured interview via telephone or the audio feature on Zoom videoconferencing (https://zoom.us/). Telephone interviews were undertaken with the use of a hand-held recorder. Participants discussed their experiences during the first year of the pandemic by responding to questions related to 3 topics. To reduce bias, licensed health providers on the team were not involved in the consent or interview processes.
Interviews were recorded, transcribed verbatim and deidentified, then imported into NVivo 12 software. Member checking18 was achieved by providing interviewees a copy of their interview transcript and an opportunity to provide additional feedback or comments. One participant withdrew their transcript, citing lack of time to respond, and other participants provided minor feedback, mostly grammatical. Data collection continued until thematic saturation18 was achieved.19
Data analysis
The analysis was conducted by 5 members of the research team, including a postdoctoral fellow and a full professor (E.A.F., S.K.J., M.J.L., M.E. and T.L.P.), all with training and experience in thematic analysis. An a priori codebook, based on the research questions, assisted coders to organize the data.21 Four transcripts were analyzed to pilot test the codebook and refinements were made. Illustrative quotations were added to the codebook to support further organization. Each transcript was then double coded.
Thematic analysis involved identifying patterns of meaning by coding and classifying data according to themes.22,23 Developed themes were then interpreted by seeking commonalities, divergence, relationships and overarching patterns in the data. Transcripts were read and reread as data were extracted and organized into the codebook. Next, the organized data were analyzed, and themes related to the objectives and supported by interview data emerged. Coding team members met regularly to review the organized data, develop codes, discuss generated themes and reflect on their collective judgments and belief systems. On 2 occasions, emerging themes were presented and discussed by the full research team. Discrepancies were resolved as a team, through discussion. Reflexivity was addressed by also discussing how team member roles, experience, perspectives and relationships may be influencing the analysis. Saturation occurred when participant responses were repetitive to those of previous participants and no new insights were revealed.
Ethics approval
The study was approved by the Nova Scotia Health Research Ethics Board (NSHA REB ROMEO file no. 1025661).
Results
Twenty-four primary care providers were interviewed (Table 1); 1 participant withdrew their data owing to lack of time to review their transcript. To preserve anonymity in a small province, participants are described simply by discipline, geographic area of practice and years of experience. Interviews averaged about 40 minutes in length; all but 1 were conducted by videoconferencing. Although family physicians, nurse practitioners and family practice nurses experienced their roles differently, their reports are combined, as they had similar responses.
Participant characteristics*
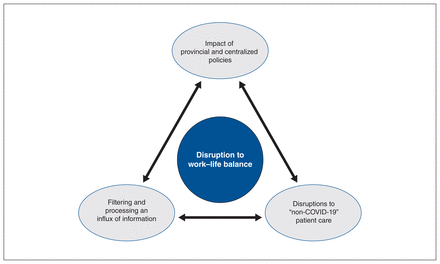
Four interrelated themes were identified within the data: disruption to work–life balance, disruptions to “non-COVID-19” patient care, impact of provincial and centralized policies, and filtering and processing an influx of information.
Figure 1 was constructed through several discussions among research team members of the results and how the themes relate to each other. There was a consensus that the theme of disruption to work–life balance was a central component of the primary care providers’ experience during the early waves of the pandemic. The disruption to work–life balance is centralized in Figure 1 also to highlight the interconnectedness of the themes, and the direct and foundational influence on primary care providers’ personal lives. The bidirectional arrows highlight the interaction observed between themes.
Impact of the COVID-19 pandemic on family physicians, nurse practitioners and family practice nurses.
Disruption to work–life balance
It’s just — it’s stressful. I don’t know if you feel like you fully get a break sometimes. (NP1)
Participants described disruption to their work–life balance during the first months of the COVID-19 pandemic, characterized by increased burden in both home and work roles, and coupled with feelings of isolation (Box 1). Multiple factors contributed to the imbalance, including changes in professional roles and responsibilities, changes in work location and increased overall stress. The closure of schools and child care programs created disruptions to everyday routines for providers with children. Many reported seeking child care assistance from family members and friends, which allowed them to “see” patients, often from home.
Disruption to work–life balance — illustrative quotations
Shift in work–life balance
They [kids] basically just really had to fend for themselves within the house and had to be quiet while Mommy was on the call with patients and so, you know, tablets, iPad, TV, a lot of that stuff which still gives me — that I’m really still upset about. (FPN1)
I have a husband who is one of those folks with chronic conditions and so, absolutely, I was the huge risk of the house. I’m in the hospitals, I am in the evening walk-in clinics, I am in the office … we very quickly separated our house into an upstairs/downstairs … . We meet at opposite ends of the dinner table for a break time and then go our separate ways again. (FP1)
Physical isolation
The day we were told that everything was shutting down, in my personal life I said, “Husband, I’m moving to the spare room. I’ll have the spare bathroom. You’re over there.” I said, “And I’ll come out when we slowly start to reopen.” So, for 3 months I slept separately from my husband in case I was exposed. (NP2)
Social isolation
I found, like, nobody else really got it. Like, even if I would talk to my friends and I would kind of be like, huffing and puffing and they were always trying to be optimistic … I was just like, oh, I give up, like, talking to you guys. Like, people just really didn’t know. (NP3)
For those who continued to work in clinical environments with high risk to SARS-CoV-2 exposure, concerns for the safety of family members created additional anxiety and stress. Providers described putting in place physical precautions to prevent transmitting the virus to their family members. These included removing clinical or hospital clothes and showering before greeting family or staying physically removed from family altogether. Feelings of isolation were exacerbated by social situations when family and friends did not understand the severity of the pandemic. Owing to this lack of understanding, many participants felt that they were unable to share their fears and concerns.
Disruptions to “non-COVID-19” patient care
People were just terrified. They didn’t want to come in. They didn’t want to be seeing me for their medications, for their blood work, even if it was necessary blood work. (NP4)
Primary care providers voiced deep concern about the long-term impact of the pandemic on the health of individuals and the health care system. Specifically, these included delayed non-COVID-19 patient care and the pressure on health system capacity (Box 2). Although services became more available after the first few months, participants observed that many of their patients continued to hesitate to seek care, and they worried that patients’ conditions would worsen as a result.
Disruptions to “non-COVID-19” patient care — illustrative quotations
You don’t realize until all you have is a phone call that a great deal of your assessment is actually done as the patient walks up the hall with you … a lot of it is visual. (NP5)
I think the downfall for COVID has been with blood pressure and prenatal for family practice … . For example, if they had cramping or a miscarriage, then it was months before they were seen at the obstetrician’s office. We had 2 babies born premature, which potentially if they had been followed more often this may not have happened. This was an unexpected issue. (FPN2)
We might be preventing COVID, but what are we going to miss in the meantime … what about my senior citizen who now is, like, has a sugar of 26 and is not coming in. (NP3)
My biggest challenge was getting interventions, so diagnostic interventions for my patients. I needed to contact the physician on call in the emergency department, have the person go to the emergency department to be assessed by the physician. (NP6)
Impact of provincial and centralized policies
The problem with primary care in Nova Scotia is that a lot of policies and a lot of the decisions are made based on how primary care looks in the city. (FP2)
Participants described 2 important impacts that occurred during the pandemic, both of which arose from implementation of provincial policies: the pivot to virtual care (Box 3) and challenges faced by rural clinics (Box 4).
Pivot to virtual care — illustrative quotations
Benefits
It would be a real shame if some of that innovation such as virtual care will not be carried forward. (FP3)
People are pumped. People have wanted this [virtual care] for a long time, I think, and are quite happy to do it … I find a lot of people are really happy to be able to access care and not have to come in, you know, they don’t have to take half a day off work … I’ve discussed it with management a few times. I really would like to keep it. (NP7)
There are many appointments that we could do virtually, and I do believe that it is time-saving, it is cost-saving, it provides better patient and provider satisfaction. (NP6)
Simplifying and understanding virtual care
I think systemic challenges, I would hope that if virtual care is okay going forward that it wouldn’t be mired in issues that make the utility lower in terms of, like, increased paperwork, et cetera. I would hope there would not be aggressive auditing, punitive auditing processes of the visits. (FP3)
I think the health authority — I think they play a really important role in helping us with that education campaign on the importance of — for the patients, the importance of realizing that virtual care is no less important and no different than in-person care. (FP1)
Challenges with virtual care
I work in an area where we have an older and less affluent population. A lot of the population don’t actually have access to — they’re still using flip phones, if they even have phones … . It was really kind of a sad thing to see and a big challenge for me to try and help them when I still also said, “you can’t go anywhere,” but here’s some medication and here’s some supports you can’t access because you don’t have a computer. (NP9)
Unique needs of rural communities — illustrative quotations
Impact of policies on rural clinics
… if I have to quarantine, what do I do? And the answer from higher up was always, well find someone to cover your practice … in places rurally, like in some of our communities we have 2 doctors doing everything, so you can’t just say, “find someone to cover your practice.” (FP2)
Characteristics of rural populations
Well, you know, what they weren’t taking into consideration is that many people in rural areas don’t have great Internet service so getting onto a website, particularly since libraries were all shut down and for some that was their only means to actually get online. (FP4)
… we serve [rural], which is demographically very different than, let’s say, the Central Zone where … . A lot of our patients don’t have the Internet. A lot of our patients don’t have vehicles. A lot of patients live in poverty, and so guidelines and kind of expectations put out by the health authority about providing care look really different here than they do in [urban area]. (FPN3)
The pivot to virtual care
In response to provincial public health policies, all primary care providers increased use of virtual care. Simplified billing for virtual care for family physicians, either by telephone or video conferencing technology (i.e., Zoom for Healthcare), was approved by the province of Nova Scotia. Providers highlighted and welcomed the adoption of virtual care, emphasizing the need to maintain virtual care postpandemic as an effective health care option for patients (Box 3). Primary care providers discussed the benefits of virtual care, describing how they directed patients to either in-person or virtual visits over the telephone. This enabled effective use of their limited hours for in-person care and related time-savings for their patients and themselves.
Despite the positive response to virtual care, participants identified challenges related to the high reliance on the Internet and technology. Providers reported that their patients, and they themselves, had challenges accessing or working with the technology associated with virtual care. Internet bandwidth and virtual care setup were frequently mentioned challenges. Access to and affordability of necessary equipment were additional challenges, particularly in rural areas.
Unique needs of rural communities
Participants working in rural communities described how top-down policies, enacted to mitigate the spread of SARS-CoV-2, were primarily designed for primary care providers and clinics in the urban centre (Box 4). For example, family physicians described how policies designed to meet the needs of solely office-based practitioners were less applicable to those in rural areas, who frequently worked in multiple locations (e.g., primary care office and emergency department). To avoid virus transmission, primary care providers were restricted to a single work setting, which created staffing challenges in areas that rely on mobility of a small number of staff.
Filtering and processing an influx of information
There’s no human way to keep on top of all of this. (FP5)
Participants described a fear of missing important policy or procedural changes and the need to develop new strategies to efficiently review and manage the most relevant information (Box 5). They scanned information for pertinent changes to rules and regulations and directed attention to profession-specific information. They also compared knowledge with colleagues to confirm what they gleaned. These strategies were an attempt to deal with the overwhelming amount of information being shared and a fear of missing important policy or procedural changes.
Filtering and processing an influx of information — illustrative quotations
Too much information, not enough time
If it was too much information you would just, you know, sift through and delete what was not relevant to you and then you would keep what was relevant to you. (NP6)
I didn’t have enough time in my day to keep up with all the information … it was just that ever-changing update that I found difficult … I got nervous for a little while about missing other things. (NP3)
I think one of the problems was, not problems but challenges, there was such a large volume of communication and such rapidly changing rules that a lot of doctors felt really confused. (FP2)
Misinformation
It’s the confirmation bias thing, right? Like, you read a story somewhere and it’s, well obviously the oxygen issue is the problem because that’s how I feel. I feel like I can’t breathe. So, there’s like a banging your head against the wall type of education that you have to provide, where it doesn’t really matter what you say, people have already convinced themselves that they don’t want to do it. (NP7)
While struggling themselves to maintain currency amid the rapidly changing science, primary care providers also discussed their need to disseminate information to patients in response to confusion caused by misinformation. For example, mask use was frequently discussed with patients owing to misinformation regarding use and importance. Primary care providers noted their increased role in patient education and reassurance during the pandemic to counter outdated or incorrect information.
Interpretation
The COVID-19 pandemic has transformed how the primary care system functions.7,24 Our results highlight multiple impacts that public health policies and regulations, enacted to mitigate and prevent the initial spread of SARS-CoV-2, had on primary care providers in Nova Scotia during the first phase of the pandemic. Disruptions to providers’ work–life balance and to non-COVID-19 patient care, and the constant filtering and processing of information influenced primary care providers’ experience and delivery of care.
Our results join with those of others25,26 in supporting tailored policies to each community’s unique characteristics and needs,25 particularly the needs of low income or rural populations. Primary care providers reported that provincial policies were insufficient in accounting for organizational and patient differences between communities and clinics during the pandemic. An example of this challenge was the province-wide adoption of virtual care.27 About 75% of participants from rural areas reported that patients had challenges or were unable to access the Internet or technology for virtual care, meaning many patients went without care.27 Many others reported that the pandemic has not affected all groups evenly: greater impacts have been observed in groups with preexisting vulnerabilities and Indigenous populations — both of which are more likely to live in rural areas.28,29 Pandemic and emergency management policies must address differential needs of populations at risk to redress inequities. Other researchers concur, reporting that rural communities have had difficulty addressing surge capacity during the pandemic due to staff or funding shortages.30 We thus conclude that the application of the same policies across all regions during a pandemic has detrimental consequences for patients, particularly the most vulnerable. Given the research evidence calling for measures to reduce inequities in digital health training and policies,31 we further suggest that health system solutions enacted in response to public health measures be tailored to local contexts.
Despite its challenges for rural providers and patients, virtual care has demonstrated its potential during the pandemic by decreasing emergency department visits, preserving resources and slowing the spread of SARS-CoV-2.32,33 It is unlikely that virtual care will cease; instead it is likely to spread,34 in which case custom solutions for rural populations are critical. One Nova Scotia solution to address inequities in access to virtual care is the “virtual library” initiative, which provides patients access to virtual care within a private space at their local library.35 This initiative has been positively received by users.36 Similar programs will be important for jurisdictions planning to expand virtual care.
A critical goal of the immediate pandemic response was to preserve the capacity of the health system, hence the enactment of policies and procedures to reduce and restrict nonessential health services.37 As a result, many patients, including people with chronic conditions, mental illness and health care hesitation due to the pandemic,7,28 lacked regular access to care for extended periods. Primary care providers in this study described consequent harmful impacts on patients, including considerable unforeseen consequences of physical closure of offices and restricted access to primary care. On the basis of this study, and in concert with others,38 we propose that primary care systems be equipped with specific primary care pandemic response plans that would not only provide ongoing access to patients, but also mitigate the impact of public health crises by attending to patient needs in the community, thereby offsetting pressures on hospital care.
In response to the COVID-19 “infodemic,” we also suggest that pandemic response plans incorporate messaging tools for primary care providers to use in future pandemic or emergency situations.39 Participants in this study reported an increased need to attend to patients who were overwhelmed and confused, which was caused by the excessive amount of misinformation, through regular interactions and discussion. Providing appropriate and accessible methods of effective patient communication to primary care providers during times of increased informational challenges has potential to reduce harm, both for patients and primary care providers. Furthermore, given that participants described challenges in reviewing the plethora of information being disseminated throughout the pandemic, there is a need to ensure information is disseminated concisely and tailored to specific professions.
Continued research is needed to enhance system resilience and recovery from the current pandemic and to prepare for future public health crises. Many primary care providers implemented creative changes to their clinics and offices, while others, particularly women, were challenged to find new ways to balance home and office. These difficulties with work–life balance were further strained by the social and physical isolation experienced by many primary care providers caused, in part, by safety concerns for vulnerable family members. Further research is required to develop supportive policies designed with the flexibility needed to meet the local needs of patients and providers. Finally, evidence that supports effective system-wide policies that accommodate new ways to achieve work–life balance, reduce feelings of isolation and address gender equity appear critical for the primary care system to emerge from the pandemic better prepared for times of crisis.
Limitations
Strengths of this study include the composition of the research team (patient advocate, health authority directors, administrators and clinicians) and the rigorous efforts made to ensure trustworthiness (credibility, confirmability, dependability and transferability) of study findings. However, this study explored the experiences of family physicians, nurse practitioners and family practice nurses, limiting the transferability of results to patients, health administrators and other primary care providers. Research that includes and compares experience across multiple disciplines may uncover new insights. Further, while all participants were asked to reflect on their experience during the very early months of the COVID-19 pandemic, participants interviewed later in the study may have experienced recall bias. They may also have been able to look back on that time with a deeper understanding of the pandemic, potentially providing more reflective responses.
The research team acknowledges that, as a mix of researchers, managers and health professionals, we have biases that may have influenced interpretations and analysis. We mitigated this risk through our interdisciplinary approach to the analysis and team discussions and consensus. Additionally, despite providing participant confidentiality throughout the process, we acknowledge that social desirability bias exists during participant interviews, which may have influenced some responses.
We theorize that our challenges to recruitment for this study were due in part to COVID-19-related pressures on eligible primary care providers, in that the providers were dealing with too many personal and profession pressures to respond to our recruitment in a timely fashion. This is also reflected in their responses to study questions and further highlights the impact of the pandemic on their day-to-day lives. Slow recruitment was also due to the departure of research team members responsible for recruitment and coordination. These team members left to pursue alternative career paths.
Conclusion
The COVID-19 pandemic has presented challenges to the primary care system and workforce. Finding ways to manage the crisis and its accompanying stress and workload will require coordinated efforts and new ways of working, balancing professional and personal life, and adapting to already implemented changes (i.e., virtual care). A specific primary care pandemic response plan could mitigate the challenges imposed on the overall system by public health crises.
Acknowledgement
The authors acknowledge the work done by research and patient representative Kylie Peacock for contributing to the study’s data collection and protocol design.
Footnotes
Competing interests: None declared.
This article has been peer reviewed.
Contributors: Tanya Packer and Jeanna Parsons Leigh conceived and designed the study. Mark Embrett, Tanya Packer, Emily Fitzgerald, Sabrena Jaswal, Michelle Lehman, Marion Brown, Fred Burge, Erin Christian, Jennifer Isenor, Emily Marshall, Ruth Martin-Misener, Tara Sampalli, Joanna Zed and Jeanna Parsons Leigh contributed to recruitment and acquisition of data. Mark Embrett, Tanya Packer, Emily Fitzgerald, Sabrena Jaswall and Michelle Lehman led the analysis and interpretation of data, and drafted the manuscript, which all other authors revised. All authors gave final approval of the version to be published and agreed to be accountable for all aspects of the work.
Funding: This work was supported by the Canadian Institutes of Health Research Canadian 2019 Novel Coronavirus (COVID-2019) Rapid Research Funding Opportunity – Operating Grant (grant no. RN420046-439965). The funders had no role in study design, data collection and analysis, decision to publish or preparation of the manuscript.
Data sharing: The data set is held securely at Dalhousie University. The data are not available for use other than for the current research project. Only individuals approved through the Dalhousie Office of Research Services may access the confidential data.
Supplemental information: For reviewer comments and the original submission of this manuscript, please see www.cmajopen.ca/content/11/2/E274/suppl/DC1.
This is an Open Access article distributed in accordance with the terms of the Creative Commons Attribution (CC BY-NC-ND 4.0) licence, which permits use, distribution and reproduction in any medium, provided that the original publication is properly cited, the use is noncommercial (i.e., research or educational use), and no modifications or adaptations are made. See: https://creativecommons.org/licenses/by-nc-nd/4.0/
References
- © 2023 CMA Impact Inc. or its licensors